【Major points】
- Hospice palliative care is actively deal with your or your family's physical, psychological, and mental symptoms.
- Hospice palliative care provides physical symptom control and psychological support.
- Hospice palliative care provides you or your family with a better quality of life.
- For more information, please go to the family medicine clinic.
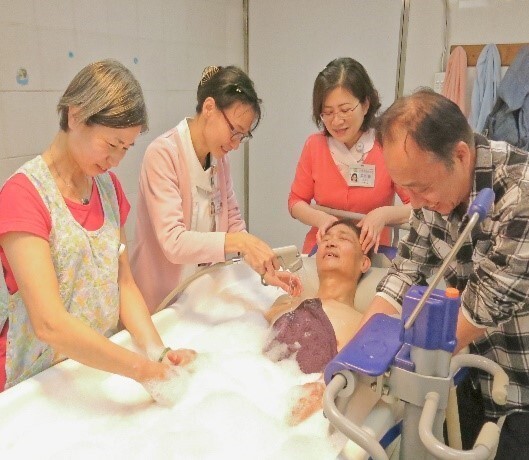


What is hospice palliative care?
Hospice palliative care aims to provide active and holistic care to end-stage patients who do not respond to curative treatments. The professional medical team invite the patient and their families to participate in the care program to enhance the dignity of life and a good quality of life without regrets.Who can receive hospice palliative services in Taiwan?
- Terminal cancer patients.
- Terminal illness including motor neuron atrophy, senile and early age organic psychosis (dementia), heart failure, respiratory failure, renal failure without dialysis or cessation of dialysis, liver cirrhosis, etc.
- Myelodysplastic syndromes (MDS)、terminal frailty in old age.
- Rare diseases or other life limits are estimated.
- Meet the clinical conditions listed in
the law on Patient Right to Autonomy Act ,Article 14,Paragraph 1,Paragraphs 2 to 5 , such as:
- The patient is terminally ill.
- The patient is in an irreversible coma.
- The patient is in permanent vegetative state.
- The patient is suffering from severe dementia.
- Other disease conditions, announced by the central competent authority, that shall meet all of the following requirements that the conditions or sufferings are unbearable, that the disease is incurable and that there are no other appropriate treatment options available given the medical standards at the time of the disease’s occurrence.
What services can hospice palliative care provide?
- The hospice palliative care team works with you or your family to develop a care plan
- To control physical discomfort symptoms such as pain, breathing difficult, nausea and vomiting, bloating and constipation, wound care ,etc.
- Provide comfort care teaching, such as: body cleaning, turning position, etc
- To integrate psychological and spiritual needs into medical care programs.
- Guide family members to accompany them at the end of life.
- To assist patients and families to face the final stages of life and adapt to the process of bereavement.
- Connecting hospice home care, hospice shared care and hospice palliative care consultation.
References
- Alshakhs, S., Park, T., McDarby, M., Reid, M. C., Czaja, S., Adelman, R., Sweet, E , Jedlicka, C. M., Delgado, D., & Phongtankuel, V. (2024). Interventions for family caregivers of patients receiving palliative/hospice care at home: A scoping review. Journal of Palliative Medicine, 27(1), 112-127. https://doi.org/10.1089/jpm.2023.0160
- Fu, F., Ng, Y. H., Wang, J., & Chui, E. W. T. (2024). Journey to inpatient hospice care: A qualitative study on the decision-making process of Chinese family caregivers of persons with terminal cancer. Patient Education and Counseling, 119, 108072. https://doi.org/10.1016/j.pec.2023.108072
- Taipei Veterans General Hospital Cancer Committee Cancer Hospice Care Group (2022). Taipei Veterans General Hospital Hospice and Palliative Medicine Manual, Taipei: Taipei Veterans General Hospital.
Quiz
Please answer the following questions:
Nursing Instruction Satisfaction
The statistical results are not open to the public.
Please log in to rate
- Location
-
- Category
- Health Promotion